Report: Inmates Denied Drug Replacement Therapy
PROVIDENCE, R.I. — Many state prison inmates with substance-abuse problems are denied access to drug replacement therapy, which is one of the most effective ways to treat heroin and opium addiction, according to a recent study.
Only 28 of the 49 correctional departments surveyed for the study offer opiate replacement therapy using methadone or buprenorphine, according to researchers from Miriam Hospital and Brown University. Even in systems where ORT is available, it is often provided under limited circumstances, with roughly half of the states limiting the use of ORT to pregnant inmates, researchers say.
 |
More than half of inmates in the United States have a history of substance abuse, according to experts. Some 23 states, or about 45 percent, provide continuity-of-care referrals to ensure that released offenders have access to methadone as they transition back into the community, while 15 states, or about 30 percent, provide referrals for buprenorphine.
“Both the World Health Organization and the Center for Disease Control recommend that prisons make these drugs available to inmates,” says Amy Nunn, the study’s lead author and an assistant professor of medicine at Brown’s Warren Alpert Medical School.
Methadone is used for the treatment of opiate dependence because of its ability to prevent withdrawal symptoms and drug cravings, as well as its success in reducing the risk of relapse and infectious disease transmission. Buprenorphine is a newer opiate treatment drug with less risk of overdose.
“In spite of these national and global recommendations that prisons provide these drugs, prison systems simply are not providing inmates with essential medicines, and that is a violation of their human rights,” Nunn says.
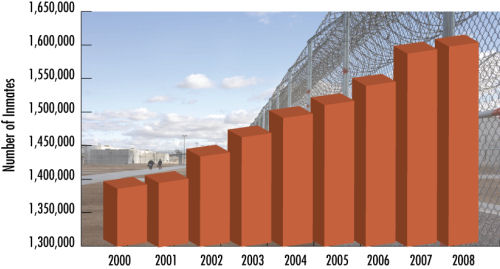
The number of prison inmates with substance-abuse problems has skyrocketed in the last 30 years, with sentencing laws for drug-related crimes serving as one of the primary drivers behind the trend, Nunn says. Failure to treat addiction creates additional problems — including needle sharing, which increases the spread of infectious diseases such as HIV/AIDS — and higher recidivism rates.
Because of the stigma of treating drug dependence with more drugs, prisons will often employ drug-free detoxification approaches and peer-based counseling support such as Narcotics Anonymous programs. Inmate addicts should have access to an array of treatment options, including ORT, to most effectively treat the problem, Nunn says.
Researchers found that some prison directors have regressive views on opiate drug treatment methods, Nunn says, while others see the importance but can’t get the support of administrators to implement an ORT program. Some directors have security concerns over providing inmates with methadone and buprenorphine as well.
The study also emphasized the need for prison systems to provide a link to community care services, so that when inmates are released, they can get access to addiction treatment programs and peer support groups. Inmates are most likely to relapse into substance abuse immediately after they are released, Nunn says.
 |
|
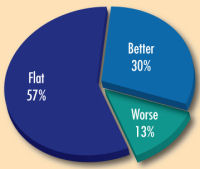
Almost 90 percent of architects in the justice sector anticipate improvement or stability in the justice design and construction market in 2010, according to a Correctional News survey of almost 800 design professionals from the justice sector. Only 13 percent of survey respondents foresee further
contraction of activity.
Source: CN Infometrics readership survey of justice sector architects |
Researchers undertook the nationwide survey through a qualitative questionnaire administered to the Federal Bureau of Prisons, the department heads of 49 state correctional systems and the District of Columbia. North Dakota refused to participate in the study, which was carried out in association with the Center for Prisoner Health and Human Rights, a nonprofit advocacy group.
“We undertook this study because there are about 200,000 people who cycle through the prison system every year who have opiate dependence, and most of them don’t have access to addiction treatment services,” Nunn says.
The research was supported by grants from the National Institutes of Health’s National Institute on Drug Abuse and Center for AIDS Research, with the study published in the medical journal Drug and Alcohol Dependence.






